Medicare Advantage Enrollment Periods: When can I enroll – 2025?
UPDATED Nov. 23, 2025. You may join, switch, or drop Medicare Advantage Plans only during Medicare Advantage Enrollment Periods. People who either have Medicare and Medicaid or qualify for Extra Help are an exception to this rule because they can switch plans every month.
Medicare Advantage enrollment is on a calendar year basis, starting the date your coverage begins.
Annual Election Period – Liberty Medicare Library
Article Contents
Initial Enrollment Period (IEP)
Initial Coverage Election Period
Medicare Open Enrollment Period
Initial Enrollment Period (IEP)
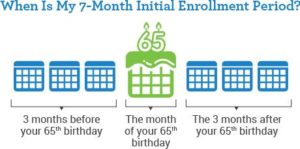
The Initial Enrollment Period (IEP) is a 7-month period that begins 3 months before you turn 65 or 3 months before your 25th month of disability. It is used to enroll in Medicare Part C and Medicare Part D and includes the 3 months before, the month of, and the 3 months after the triggering event, such as turning age 65.
Initial Coverage Election Period (ICEP)
The Initial Coverage Election Period (ICEP) is either 3 months or 7 months. ICEP ends either the last day of the month before you are enrolled in both Parts A and B, OR the last day of the IEP – whichever is later. Therefore:
- If you are new to Medicare and signed up for both Part A and Part B during the IEP, then ICEP is identical to IEP and lasts 7 months
- If you have delayed Part B enrollment, then ICEP lasts 3 months and ends before you are enrolled in both Parts A and B. In other words, ICEP ends just before your Part B begins. This is obviously very confusing – please contact us for clarification.
If your plan becomes effective, you may not make another ICEP election even if the ICEP has not expired.
Read also: Initial Coverage Election Period (ICEP) and delayed Part B enrollment.
Medicare Open Enrollment Period
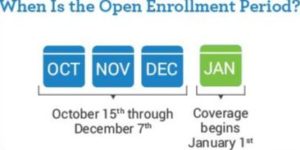
The Medicare Open Enrollment Period, also known as the Annual Election Period (AEP), runs from October 15 to December 7. Your coverage will begin on January 1 of the following year. You may switch between Medicare Advantage plans. You also may change from the Medicare Advantage plan to Original Medicare, or from Original Medicare to the Medicare Advantage plan. You also may change the Prescription Drug Plan (PDP), enroll in it (if you didn’t have it), or disenroll from it.
Notice, if you are in the Medicare Advantage plan with Prescription Drug Coverage (MAPD), and you decide to join the stand-alone Medicare Prescription Drug Plan (PDP), you’ll be disenrolled from your MAPD plan and return to Original Medicare.
You may make more than one election during the AEP. Your final election during that period is the one that counts.
Medicare Advantage Open Enrollment Period (OEP)
The Medicare Advantage Open Enrollment Period (OEP) runs from January 1 to March 31. It allows people enrolled in an MA or MAPD plan to make a one-time election to switch to another Medicare Advantage plan, or to leave their Medicare Advantage plan and return to Original Medicare, with the Medicare Part D plan. It does not allow for changes in stand-alone PDPs.
You can only make ONE change during this period.
Special Enrollment Period (SEP)
In certain situations, you may be eligible for a Special Enrollment Period (SEP), which allows you to make changes in your coverage outside of Medicare Advantage enrollment periods described above. Examples of SEP include:
- You’ve moved out of the service area
- You are disenrolled from an employer/union group health plan
- You are qualified for an Extra Help or State Pharmaceutical Assistance Program (SPAP)
- You have both Medicare and Medicaid
- You are enrolling in the 5-star plan, etc.
US Government Sources
Let Liberty Medicare Help You
If you are looking for Medicare Advantage coverage, Liberty Medicare is here to assist you. We’ll help in all stages of comparing, selecting and enrolling in the best and most suitable Medicare Advantage Plan for you. Our services are offered at no cost to you.
Learn more about all the benefits of working with Liberty Medicare.
Contact us with your Medicare Questions, or give us a call at 877-657-7477, and you will be connected to a licensed agent/broker.





